WHAT IS A DEEP VEIN THROMBOSIS (DVT)?
Deep Vein Thrombosis (DVT) occurs when a blood clot (thrombus) develops in one or more of the deep veins of the legs, pelvis, or arms. Blood clots can form in either superficial veins (known as superficial thrombophlebitis) and/or in the deep veins. Blood clots in superficial veins rarely cause serious problems; however, clots in the deep veins require immediate medical attention.
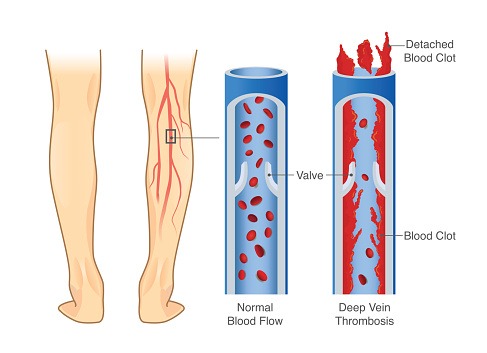
Veins located deep in the center of the leg are surrounded by strong muscles. When they contract, they force deoxygenated blood back to the lungs and heart. In a healthy vessel, one-way valves prevent the backflow of blood between the contractions. Through repeated contractions, the blood is ultimately returned from the legs to the heart. The development of clot in the legs can result in serious morbidity and can even be fatal. Clots in the legs can break off and travel through the bloodstream to the heart and lungs as a pulmonary embolism (PE). Large pulmonary emboli can cause critical strain on the heart, resulting in cardiac arrest. Beyond the risk of migration, thrombus in the legs can cause severe swelling and pain in the leg, which can be permanent. In rare cases, the clot itself can threaten the viability of the affected limb.
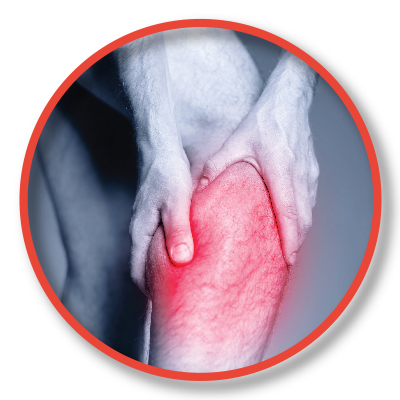
WHAT ARE THE COMMON SYMPTOMS OF DVT?
- Warm feeling in the affected limb
- Discoloration of the skin (blueish or reddish)
- Distension of superficial veins at the skin
- Swelling
- Pain or tenderness in the affected limb when pressure is applied
WHAT ARE THE RISK FACTORS ASSOCIATED WITH DVT?
Blood clots in deep veins can develop when the circulation of blood slows down due to injury, illness, or inactivity. Blood can accumulate or “pool,” leaving a perfect setting for a clot to form.
Risk factors for DVT include:
- Obesity
- Coagulation abnormalities
- Injury to the lining (endothelium) of the veins
- Previous or current cancer
- Inflammatory diseases and some autoimmune diseases
- Pregnancy or post-partum
- Hormone therapy or oral contraceptives
- Over the age of 40
- Recent injury of surgery
- Antiphospholipid syndrome
- Immobility, such as bed rest or sitting for extended periods of time
- Previous or family history of DVT
- Smoking
- Heart failure
- Infection
- Polycythemia vera
- Nephrotic syndrome
- HIV
- Chemotherapy
- IV drug use
- Foreign bodies (e.g., central venous catheters)
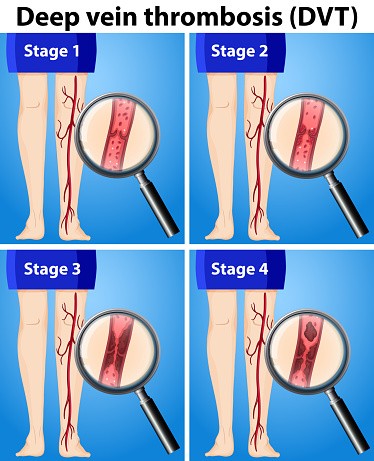
WHAT ARE THE STAGES OF DEEP VEIN THROMBOSIS?
This next photo visually depicts the narrowing of blood vessels overtime in the deep veins.
Our providers are nationally recognized as experts in minimally invasive therapies for treating DVT.
We provide treatment for DVT for patients throughout Western, MA and Northern, CT.
To learn more about treatments available at New England Endovascular Center call 413-693-2852 to make an appointment.
